Ayushman Bharat: The world’s largest national health protection scheme leveraging digital health towards achieving UHC in India
With the largest UHC and digital health programmes in the world, India’s experiences offer significant learnings for the rest of the world.
On 23 September 2018, India launched the world’s largest universal health coverage (UHC) scheme named Ayushman Bharat Pradhan Mantri- Jan Arogya Yojana (AB-PMJAY), which intended to cover 500 million Indians in the bottom 40 per cent of the Indian population. The scheme provides cashless cover of up to INR 500,000 to each family for secondary and tertiary care hospitalisations. Safeguarding that primary health care is not left out, the scheme also proposes establishing 150,000 wellness clinics by transforming existing sub-centers and primary health centres, the country’s two lowest level health facilities. Other than providing curative services, the wellness clinics will also emphasise disease prevention and health promotion. Thus, AB-PMJAY takes a holistic view of securing families from diseases and subsequent financial catastrophes while ensuring a sustainable UHC scheme.
Having 28 states and 8 union territories, Indian health care is devolved, and health is a state subject. Many states and union territories had their health protection schemes.Ayushman Bharat strives to and has been largely successful in unifying most schemes under one umbrella, thereby promoting a one-nation-one-UHC model.
There were many precursors to AB-PMJAY, such as Employees State Insurance, Rashtriya Suraksha Bima Yojana, Central Government Health Scheme, and a few others. AB-PMJAY is different from its precursors on several measures, the most important of them being the robust digital architecture that complements the scheme. An extensive provider-linked information system has been created to make payments. Also, the technology platform leverages artificial intelligence and machine learning to prevent abuse and control fraudulent transactions.
India has a long history of digital health initiatives, including telemedicine and e-pharmacies, though they have been sporadic and uneven. The National Health Policy 2017 emphasises citizen centricity, quality of care, better access, UHC and inclusiveness as some of the core principles of Indian health care. Technology is a critical component that can help realise these principles; however, an interoperable enterprise-level federated digital architecture was necessary to bridge the gaps and make the system even, especially considering the diversity and complexities of the Indian health system.
The NDHB (now ADBM) Architecture
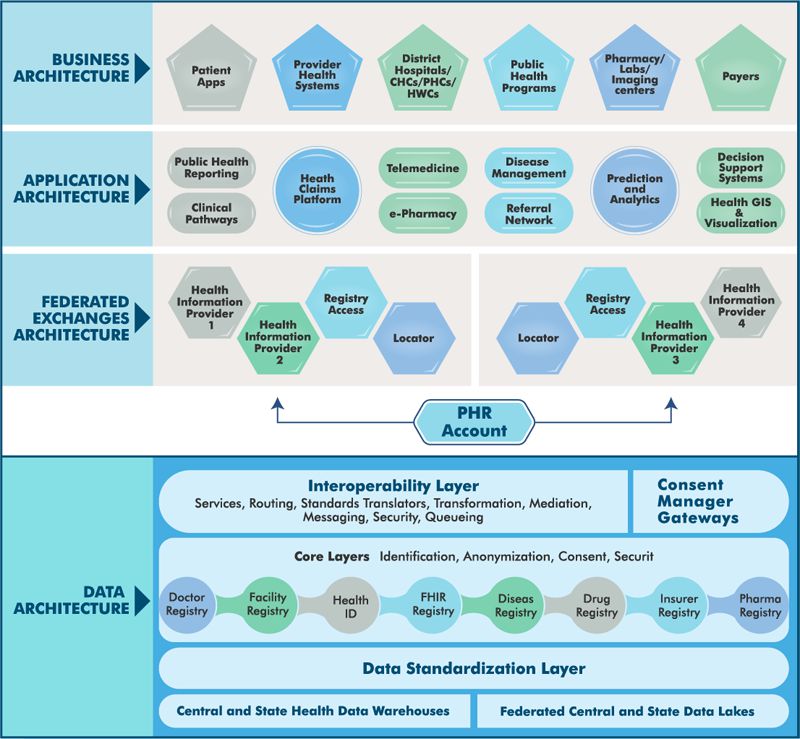
The above needs led to the development of the National Digital Health Blueprint (NDHB), a layered framework with a set of core principles surrounded by other layers relating to digital health infrastructure, data hubs, building blocks, standards, and regulations. The blueprint also included an institutional framework and a high-level action plan for its implementation. The blueprint has 35 building blocks, some of which consists of the following critical capabilities.
● Identification – Every citizen will have a unique health ID and access to a health locker enabling access to their health records from anywhere, thereby ensuring continuum of care. The blueprint also has a health care provider registry, a comprehensive collection of all health care professionals and facilities in the country. The beneficiaries and providers can self-enroll to create their IDs.
● Citizen Centricity – The blueprint identifies a set of building blocks that emphasises the gold standard for maintaining health records’ security, confidentiality, and privacy.
● Service Delivery – The blueprint combines web and mobile applications for delivering services on a mobile-first approach. Such applications include telemedicine and e-pharmacy.
● Interoperability – The blueprint promotes the creation of a Health Information Exchange and National Health Informatics Standards to enable interoperability.
Built on the guiding principles of “Security and Privacy by Design” and “Think Big, Start Small, Scale Fast,” the COVID-19 pandemic necessitated rapid adoption of many digital health initiatives that were part of the blueprint. The National Telemedicine Practice guidelines were released on 25 March 2020, and subsequently, eSanjeevani, the national teleconsultation service, was fast-tracked and commissioned in April 2020. eSanjeevani is now among the largest telemedicine networks in the world, and more than 14 million online consultations were conducted by October 2021.
The ADBM ecosystem
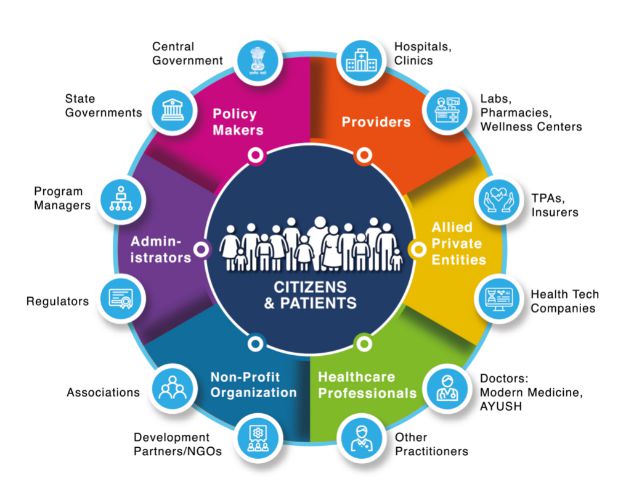
The blueprint also allows integration of all the stakeholders, a sandbox, and an API interface to integrate other private and public digital health applications. The blueprint transpired into the National Digital Health Mission (NDHM), which was piloted in 6 union territories from 15 August 2020, before it was rechristened as Ayushman Bharat Digital Mission (ABDM) and dedicated to the nation on September 27, 2021.
ABDM has been instituted with a vision to create a seamless online platform “through the provision of a wide range of data, information and infrastructure services, duly leveraging open, interoperable, standards-based digital systems” while ensuring the security, confidentiality, and privacy of health-related personal information.
By October 2021, around 168 million beneficiaries were enrolled, and AB-PMJAY had supported over 22.7 million hospital admissions. The programme achieved the milestone of 2 million hospital admissions in August 2021, and official reports indicated that the scheme had provided treatments worth more than INR 250 billion. The programme’s impact can be gauged by the fact that out-of-pocket health expenses account for nearly 63 per cent of the total health expenditure (World Bank, 2018) in India. It is also critical to note that the above volume of services was executed seamlessly through the robust information technology backbone, including the AB-PMJAY One Transaction Management System (TMS) that integrates the entire process from admission, discharges, and onwards till financial settlement.
Key lessons:
Being the largest UHC and digital health programmes globally, AB-PMJAY and ABDM foster significant learnings for the rest of the world, especially for countries with devolved health systems. Some of such learnings include-
● A comprehensive blueprint in line with the health system’s vision is quintessential for success. India has demonstrated that with a proper vision and blueprint, a lot could be achieved in a short span.
● Including primary health care – It is critical that UHC includes health promotion, disease prevention, and primary health care to ensure that people’s health care needs are met. AB-PMJAY demonstrates that a scheme favoring hospitalisation alone may not be an appropriate product for LMICs.
● Digital backbone – Digital programmes for rapid beneficiary enrollment, provider management, and delivering quality services to those deprived should be designed complementing the UHC scheme.
● Leadership – Political leadership from the top-most authority along with a multi-pronged approach is essential for rapid success.
● Organisational and operational synergy – Having UHC and digital health under the same umbrella organisation could foster synergy and rapid growth, like the case of the National Health Authority in India.
References:
1. Official website of ADBM, India; (Last accessed on 24 October 2021)
2. Media report dated 21 Sept 2021 –
https://www.business-standard.com/article/economy-policy/health-ministry-s-esanjeevani-records-14-million-consultations-121101800978_1.html(Last accessed on 24 October 2021)
3. Official Website of the National Health Authority (Last accessed on 24 October 2021)


